You must be signed in to read the rest of this article.
Registration on CDEWorld is free. Sign up today!
Forgot your password? Click Here!
Nonmaleficence is often discussed and debated in healthcare.1 No longer is it acceptable to over-prepare teeth for convenience or lack of understanding of alternative treatments. Minimally invasive dentistry is not merely a simple obligation, but a professional duty.1 The media-inspired preoccupation with looking and feeing younger obligates healthcare providers to balance ethics with literature-based information and clinical experiences to meet patient demands.2 Clinical evidence is needed to provide the standard of care required to comply with and support nonmaleficence.1,2
The concept of no-preparation or minimal-preparation veneers is more than 25 years old, yet there is no classification system categorizing the extent of preparation for different veneer treatments.2 Such a system could be indicated in various clinical scenarios and benefit dentists and patients, guiding conservative veneer preparation and placement.2
Interest in conservative treatments has increased significantly since veneering was introduced as an additive technique in the 1980s as an alternative to full-coverage crowns.3,4 Placed with little to no preparation, veneers were bonded directly to enamel on the facial surface of teeth following the conservative methods desired today.5,6 Approximately 0.5-mm thick and tapering to almost nothing at the margins, early veneers resembled those of today that have returned to more conversative varieties. Many manufacturers claim veneers can now be fabricated as thin as 0.3 mm.3
Veneers demonstrate strength, longevity, biocompatibility, and esthetics, and are also conservative. They are considered among the most viable treatments.7,8 Porcelain veneers have evolved significantly.7 Initially considered simple anterior tooth coverings, they are now treatments for various indications.7
The less clinicians invade hard tooth structure, the less likely they infringe upon and disrupt the natural barriers of the dentin-enamel junction (DEJ) and other structures. It is always preferable to end veneer margins supragingivally and preserve the cingulum and lingual marginal ridges. Comprising more than 80% of a tooth’s strength, these anatomical landmarks are significant.9,10
While conducting their studies, researchers Shillingburg and Grace found that as patients age, the enamel thickness on the facial surfaces of anterior teeth decreases.11-13 On the cervicofacial surface of the central incisor, 1 mm above the cemento-enamel junction (CEJ), enamel thickness ranges from 0.17 mm to 0.52 mm, with a mean thickness of 0.31 mm.11-13 The thickness on the midfacial surface, 5 mm from the CEJ, ranges from 0.45 mm to 0.93 mm, with a mean thickness of 0.75 mm.11-13
Overtreatment of dental hard tissues—particularly enamel—has occurred for too long. From Latin praedicius or praedicere, meaning to know beforehand, predictable suggests that dentistry should develop models that dentists can follow to provide routine comprehensive esthetic outcomes. With volumes of peer-reviewed research and documentation, enamel preservation leads to more predictable adhesive dentistry in almost all cases.
Before considering available smile-enhancing options, patients should undergo comprehensive clinical examinations, including an esthetic evaluation.14 Interdisciplinary modalities must include the following: perio-plastics, tooth bleaching, direct composite veneers, and porcelain veneers, which are options providing predictability and longevity in carefully selected esthetic cases.14 Before considering and undertaking restorative options, orthodontics should always be considered. Orthodontic treatment is a non-invasive modality for achieving desired results and/or ensuring teeth are properly positioned for long-term predictable function and esthetics. Subsequent restorative treatment using minimally invasive or no-preparation porcelain veneers can then be considered, since long-term research shows a 93% to 94% survival rate for this conservative treatment.14,15
Adhesive Dentistry: Its Influence on Conservative Esthetics
Dentistry has sound, indisputable evidence affirming adhesive dentistry as the most conservative, least invasive, and most predictable way to restore teeth to normal form, function, strength, and optical properties when tooth-colored materials are used, as well as to preserve the greatest amount of tooth structure while satisfying patients’ restorative and esthetic needs.14,16 The percentage of function achieved with tooth-colored materials compared to the amount of preparation required for conventional non-adhesive dentistry should be considered. Literature quotes percentages of restored function within a large range, from 20% to 85%.17-21 Inconsistency is explained by substrate variables, adhesive factors, and ability to control preparation design or any combination of these.17-21
The enamel bond is beyond reproach, and is the strongest, least invasive, most conservative, and most predictable bond available. Magne says it mimics the DEJ or the natural bond between enamel and dentin. The same cannot be said about bonding to the dentin. However, even bonding to dentin is favored over non-adhesive approaches.22 The “gold standard” remains total-etch three-step systems, or three-step etch-and-rinse.22-24
There remain many issues to consider before bonding to dentin.11 For example, adhesion more often fails at the dentin-cement interface.11,25 Also, microleakage typically occurs between the dentin and cement, leaving underlying dentin unprotected.11,25 Studies show that the bond strength of resin cements to dentin is much lower than bonds to enamel, which is why maintaining an enamel periphery is essential.11,25-29
Factors Affecting Tooth Preparation for Esthetic Restorations
The ideal scenario is to keep the bond completely in enamel. Of utmost importance and when properly prepared, enamel substrates provide the most predictable surface to bond porcelain.2,3,30,31 The microretentive adhesion of porcelain to enamel has been well documented for more than 20 years.2,32
Unaffected by lingual preparation design, porcelain veneers adhesively bonded to enamel demonstrate the greatest long-term success rates, making no-preparation veneers the treatment of choice when indicated.2,3,30,31 When dentin is involved, an enamel periphery is preferable for predictability.2,32 When less than 50% of enamel periphery and less than 50% enamel remain, discussion with the patient about limitations and predictability of the outcome is necessary.2,4
Despite research and many available materials, clinician experience is the most important tool for determining appropriate treatment plans to address clinical concerns and patients’ esthetic demands.2,4 To determine preparation requirements, a comprehensive clinical examination that includes function and stress analyses and an esthetic evaluation should be completed for every case.2,4,14,16,33 During the planning process, dental photographs, centric-relation-mounted study models, and other diagnostic records and factors must be considered before undertaking any procedure.2,4,14,33
When given the option, most patients choose the least amount of tooth structure removal.34 By informing patients of restorative options like porcelain veneers and resin-bonded prosthesis that only require 3% to 30% by weight loss of coronal tooth structure, dentists can provide conservative alternatives to conventional full-coverage crowns, which typically require 63% to 72% loss of structure.34 However, it is the patients’ teeth, time, and money; therefore, dentists should enable them to make informed decisions that are best for them based on prognosis, advantages, disadvantages, risks, and longevity.
Minimally invasive dentistry has new technical and educational requirements. Clinicians must stay abreast of material selection, adhesive protocol, and scientific advances. They must also understand that space requirements can greatly affect the final outcome of a finished restoration.6,35 The space often required for shade change ranges from 0.2 mm to 0.3 mm per shade.6,35 The author uses 0.3 mm plus 0.2 mm times each shade change.
Because 50% or more enamel on the tooth is required, 50% or more of the bonded substrate is on the enamel, and 70% or more of the margin must be enamel. The condition or integrity of the substrate to which veneers will be bonded is also important for success.6,9,35 Absolute isolation during cementation procedures is essential for bond maintenance, which ultimately protects the internal restoration surface and is necessary for longevity.9,35
Typical Veneer Preparation Design
Expected veneer longevity depends on tooth preparation, which should be confined to enamel and involve proximal contact areas and functional considerations, such as occlusion.36 It is also necessary to maintain the cervical enamel margin and incorporate the incisal edge to increase fracture resistance and enable proper placement.36 To increase functional and esthetic properties of restorations, proximal extensions should be created just beyond contact areas.36 The clinical success of porcelain veneers depends upon many factors. Although dental and gingival structures play important roles in optical response and withstanding masticatory forces, dentists must consider and recreate many anatomical components while providing functional integrity.36
The typical veneer preparation model is technique-sensitive and incorporates guidelines for achieving functional and esthetic results. When reducing the labial and proximal surfaces, there must be no less than 0.3 mm to 0.5 mm and uniform whenever possible.11,37-42 When going from thick to thin—as in a large Class IV incisal fracture or large Class III composite removal—a smooth transition must be incorporated. Extending the preparation interproximally to the lingual aspect of the papilla, parallel to the crown’s original form, is necessary to improve adhesion, conceal the margin, allow an accurate impression, and increase the overall veneer strength.11,39,42 The decision to reduce the incisal edge should be based on whether there is a need to increase the crown length and the labiolingual width of the incisal edge.11,39,42 Since line angles are involved, rounded corners and edges must be established.
Veneers with an incisal butt-joint or feathered edge usually demonstrate fracture loads similar to those of unprepared teeth.11,32 In these cases, the incisal edge may be reduced by up to 2 mm.11,41,43 However, the preparation’s margins must be chamfered and in enamel.11,39,41,42,44 The interproximal and gingival margins of porcelain veneer restorations also must end in enamel at or above the free gingival margin or barely within the gingival sulcus when possible.11,39,42
Techniques exist that allow for consistent tooth surface reduction while minimizing it.45-47 Because traditional veneering approaches can lead to significant dentin exposure, strategies should be taken to limit preparations to the enamel.46-48 Using an additive diagnostic procedure and silicone indexes avoids unnecessary dentin exposure, improves biomechanics and esthetics, and allows more predictable bonding.48
Defining Classifications of Veneer Preparations
Referred to as no-, minimal-, or conventional-preparation, veneer classifications—or lack thereof—create a large gray zone of misunderstanding and miscommunication with patients and within the dental profession. Left unanswered, questions regarding finish lines, tooth structure removal, and other aspects can cause confusion in practice.
Flaws and inaccuracies in previously proposed preparation guidelines make those guidelines irrelevant.49 To dissolve uncertainty, a classification system is proposed to aid with diagnosis, treatment planning, patient education, consent and understanding, and communication among dental team members, and to provide viable solutions to public requests for elective procedures.
Defined as the way something is categorized, labeled, organized, distinguished, arranged, or sorted, classification adds clarity.50 Dentistry has distinguished Class I through Class V classifications in operative dentistry; there are inlays, onlays (3/4 and 7/8), and full-coverage crowns in prosthodontics. Classifications exist for furcations in periodontics, lip lines, bone quality, LeForte’s CL-I, -II, and -III in orthodontics, removable prosthesis cantilevers, and bone/crest levels. In 1974, Talim and Gohil classified tooth cracks and fractures in endodontics, and Misch classified implant prostheses for patients; in 2009, McLaren classified ceramics.9 Since classification systems have infiltrated so many aspects of life, veneers should be no different.
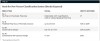
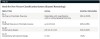
In the absence of widely advocated porcelain veneer tooth preparation guidelines, Table 1 and Table 2 show the basis for a new veneer classification system proposed by the author. The system is introduced to clarify the aforementioned gray zone between classic conventional veneer preparation and no- or minimal-preparation veneers. This metric provides an accurate measurement system for quantifying tooth structure removal on a case-by-case basis.34 Studies show that when a conservative approach is taken and significant tooth structure remains, dentists can provide patients with a better prognosis for the restored teeth.34
This classification divides preparation and veneering into reduction (referred to as space requirement, working thickness, or material room), volume of enamel remaining, and percentage of dentin exposed. Notably, classifications I, II—both of which incorporate addition veneers—and III require 70% to 100% enamel periphery.
CL-I
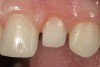
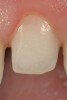
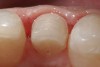
CL-I is the purest form of no-preparation or practically prep-less veneers, but can include a discreet finish line or only a loupes-detectable margin (Figure 1). The term addition veneers frequently describes this preparation design today. In this classification, 95% to 100% of enamel volume remains after preparation, and no dentin is exposed. Ideal whenever possible, preparation must be completely and only in enamel.
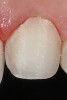
This preparation type can be easily achieved using a bis-acrylic preparation guide created from a putty or silicone matrix of the diagnostic wax-up, which can be applied to the teeth.49,50 Depth cuts of 0.5 mm for CL-I are placed into the incisal and facial aspects of the bis-acrylic preparation guide, which should result in the depth-cutting bur not touching the tooth, and the clinician should consider removing the aprismatic enamel and placing a practically undetectable finish line (Figure 2 and Figure 3) to aid ceramists in determining margin placement. These depth-cutting grooves minimize potential for over-preparation.
Many times considered the best option because of their tooth structure preservation qualities, prep-less veneers have limitations, including esthetic outcomes. Calamia found that veneers placed with no preparation resulted in periodontal problems as a result of over-contoured teeth that changed the emergence profile.2,51 It was concluded, however, that the veneer treatment modality would function long term.2,3 To correct the emergence issue, a 0.5-mm reduction restored by 0.5 mm of porcelain provided nearly the original tooth profile with the veneer in place.2 Additionally, it was discovered that wrapping the incisal edge enhances strength, and that preparations limited to the facial surface only were not as strong as those with a wrapped incisal edge.2,43 This latter veneer preparation type is described below as CL-II.
Some indications for no-prep veneers include peg-laterals, genetic anomalies producing smaller teeth, short and worn teeth, orthodontics leading to a narrow arch, and patients with larger lips. Disadvantages may include limited shade alteration capability, difficulty developing the correct axial inclination, proportional errors, and trouble forming the proper gingival symmetry.2,33
CL-II
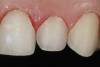
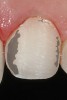
CL-II deals with minimally invasive or modified prep-less veneers (Figure 4). Addition veneers also may fall in this classification. This category should exhibit 80% to 95% volume of remaining enamel, 10% to 20% exposed dentin, and up to 0.5 mm of reduction (Figure 5 and Figure 6). Ideally, CL-II veneers would have complete enamel periphery, but may involve a small zone on the gingival margin consisting of dentin to clearly establish the restoration margins (Figure 7).52 Additionally, 5% to 15% of dentin may be exposed on any facial surface (ie, mesial, distal, or gingival), depending on veneer rotation (Figure 8). To complete a CL-II preparation, a bis-acrylic preparation guide, as previously described, can be used.
CL-III
CL-III is a conservative preparation classification (Figure 9) and described as 60% to 80% enamel volume remaining (Figure 10), 20% to 40% dentin exposed, and 0.5 mm to 1 mm of reduction (Figure 11 and Figure 12). With more room for restorative material, the gingival margin will typically involve more dentin.52 However, greater than 70% to 80% of the finish line must still be in enamel (Figure 13).
CL-IV
CL-IV is a full veneer or conventional all-ceramic design (Figure 14) and is best described as approximately 50% of enamel volume remaining, greater than 40% of exposed dentin, and 1 mm or more of reduction. The peripheral margin may consist of only 50% to 70% enamel. Although this veneer preparation type has become an almost universally accepted technique for placing full veneers, functional and esthetic limitations remain—including lower fracture loads and decreased marginal integrity that ultimately lead to restorative failure.53,54 Preparation design and fatigue influence the marginal accuracy of veneers bonded to maxillary central incisors, with significantly higher marginal gap formations developing in complete veneer preparations.53,54 Therefore, all limits of restorative options should be considered before undertaking this procedure.
Any given patient could exhibit any combination of classifications due to acidic erosion, genetics, restorative material requirements, occlusion, or tooth- and arch-size discrepancies. As in periodontics, one tooth can be a CL-I furcation and a CL-III in the same dentition, and each has differing treatment approaches, prognosis, and varying care. Again, this veneer classification system was designed to help clarify professional communication and allow patients to better understand how much tooth structure will need to be removed. Such information will enable better informed consent, with patients making the choices they see fit.
When preparations fall outside these parameters (Figure 15), a crown should be considered for predictability and longevity. It is well established that when a tooth that has greater than 50% of enamel missing (Figure 16), moderate sclerotic dentin, and greater than 3 mm of unsupported porcelain, a crown must be considered. Magne found that 65% of a tooth’s integrity comes from the cingulum and approximately 27% from lingual marginal ridges.55 These anatomical landmarks must be preserved at all costs.55 No significant differences in crown flexure were found between natural and veneered incisors when the cingulum is presevered.56
However, clinical decisions must be based on the dentist’s clinical experience, scientific data, evidence-based literature, the clinical scenario, the patient’s desires (ie, time and money considerations), and full consent based on knowledge of advantages, disadvantages, risks, benefits, and prognosis. These factors are significant in treatment selection. CL-I veneer preparation with its 100% enamel substrate is more predictable than CL-IV with its significant dentin exposure.
Conclusion
When cosmetic and adhesive procedures were initially introduced, tissue preservation was the most important goal. With recent paradigm shifts in patient desires and treatment-planning techniques, dentistry is witnessing a resurgence in conservative techniques in day-to-day practice. Although restorations need not be tooth-colored, and gold remains the best restorative material, more patients demand the esthetic potential that tooth-colored restorations demonstrate. To uphold the duty of nonmaleficence and obtain appropriate consent, dentists must still inform patients of both the benefits and consequences of choosing esthetics over function.
A paradigm shift is essential in dentistry’s current thinking regarding veneer preparations. It is no longer acceptable to limit veneer descriptions to no-prep or conventional all-ceramic designs. Proposed are two additional, distinct classifications that should aid dentists and patients in their ability to provide better communication, consent, diagnosis, treatment planning, material selection, education, and tooth structure preservation. Through the clincian’s experience and knowledge, the appropriate treatment plan can be selected based on the patient’s clinical situation and demands, to give patients the best in function, longevity, and esthetics.
About the Author
Brian LeSage, DDS
Private Practice
Beverly Hills, California
References
1. Andersson GB, Chapman JR, Dekutoski MB, et al. Do no harm: the balance of “beneficence” and “non-maleficence.” Spine. 2010;35(9 suppl):S2-S8.
2. LeSage BP. Revisiting the design of minimal and no-preparation veneers: a step-by-step technique. J Calif Dent Assoc. 2010;38(8):561-569.
3. DiMatteo AM. Prep vs no-prep: the evolution of veneers. Inside Dentistry. 2009;5(6):72-79.
4. Calamia JR. Clinical evaluation of etched porcelain veneer. Am J Dent. 1989;2(1):9-15.
5. Calamia JR. Etched porcelain facial veneers: a new treatment modality based on scientific and clinical evidence. NY J Dent. 1983;53(6):255-259.
6. Giordano R. A comparison of all–ceramic restorative systems. J Mass Dent Soc. 2002;50(4):16-20.
7. Nash R. At the chair: why conservative preparation for elective laminate veneers. Contemporary Esthetics and Restorative Practice. 2002:70-76.
8. Calamia JR. The current status of etched porcelain veneer restorations. J Philipp Dent Assoc. 1996;47(4):35-41.
9. McLaren EA, Cao PT. Ceramics in dentistry – part 1: classes of materials. Inside Dentistry. 2009;5(9):94-103.
10. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Region: A Biomimetic Approach. Chicago, IL: Quintessence Publishing; 2002.
11. Jacobson N, Frank CA. The myth of instant orthodontics: an ethical quandary. J Am Dent Assoc. 2008;139(4):424-434.
12. Shillingburg HT Jr, Grace CS. Thickness of enamel and dentin. J South Calif Dent Assoc. 1973;41(1):33-36.
13. Atsu SS, Aka PS, Kucukesmen HC, et al. Age-related changes in tooth enamel as measured by electron microscopy: implications for porcelain laminate veneers. J Prosthet Dent. 2005;94(4):336-341.
14. Strassler HE. Minimally invasive porcelain veneers: indications for a conservative esthetic dentistry treatment modality. Gen Dent. 2007;55(7):686-696.
15. Friedman MJ. A 15-year review of porcelain veneer failure—a clinician’s observations. Compend Contin Educ Dent. 1998;19(6):625-638.
16. McLaren EA, Whiteman YY. Ceramics: rationale for material selection. Compend Contin Educ Dent. 2010;31(9):666-680.
17. Roulet JF. Benefits and disadvantages of tooth-coloured alternatives to amalgam. J Dent. 1997;25(6):459-473.
18. Hickel R, Manhart J. Longevity of restorations in posterior teeth and reasons for failure. J Adhes Dent. 2001;3(1):45-64.
19. Manhart J, Chen H, Hamm G, Hickel R. Buonocore Memorial Lecture. Review of the clinical survival of direct and indirect restorations in posterior teeth of the permanent dentition. Oper Dent. 2004;29(5):481-508.
20. Fradeani M, Redemagni M, Corrado M. Porcelain laminate veneers: 6- to 12-year clinical evaluation—a retrospective study. Int J Periodontics Restorative Dent. 2005;25(1):9-17.
21. Burke FJ. Trends in indirect dentistry: 4. performance of adhesive restorations. Dent Update. 2005;32(6):312-322.
22. Van Meerbeek B, De Munck J, Yoshida Y, et al. Buonocore memorial lecture. Adhesion to enamel and dentin: current status and future challenges. Oper Dent. 2003;28(3):215-235.
23. Swift EJ Jr, Perdigão J, Heymann HO. Bonding to enamel and dentin: a brief history and state of the art, 1995. Quintessence Int. 1995;26(2):95-110.
24. Swift EJ Jr. Dentin bonding: what is the state of the art? Compend Contin Educ Dent. 2001;22(12 suppl):4-7.
25. Lafuente JD, Chaves A, Carmiol R. Bond strength of dual-cured resin cements to human teeth. J Esthet Dent. 2000;12(2):105-110.
26. Peumans M, De Munck J, Fieuws S, et al. A prospective ten-year clinical trial of porcelain veneers. J Adhes Dent. 2004;6(1):65-76.
27. Christensen GJ. Veneer mania. J Am Dent Assoc. 2006;137(8):1161-1163.
28. Hikita K, Van Meerbeek B, De Munck J, et al. Bonding effectiveness of adhesive luting agents to enamel and dentin. Dent Mater. 2007;23(1):71-80.
29. Ibarra G, Johnson GH, Geurtsen W, Vargas MA. Microleakage of porcelain veneer restorations bonded to enamel and dentin with a new self-adhesive resin-based dental cement. Dent Mater. 2007;23(2):218-225.
30. LeSage BP. Minimally invasive dentistry: paradigm shifts in preparation design. Pract Proced Aesthet Dent. 2009;21(2):97-101.
31. Magne P, Douglas WH. Porcelain veneers: dentin bonding optimization and biomimetic recovery of the crown. Int J Prosthodont. 1999;12(2):111-121.
32. De Munck J, Van Landuyt K, Peumans M, et al. A critical review of the durability of adhesion to tooth tissue: methods and results. J Dent Res. 2005;84(2):118-132.
33. Javaheri D. Considerations for planning esthetic treatment with veneers involving no or minimal preparation. J Am Dent Assoc. 2007;138(3):331-337.
34. Edelhoff D, Sorensen JA. Tooth structure removal associated with various preparation designs for anterior teeth. J Prosthet Dent. 2002;87(5):503-509.
35. McLaren EA, LeSage BP. Feldspathic veneers: what are their indications. Compend Contin Educ Dent. 2011;32(3):44-49.
36. Mangini F, Cerutti A, Putignano A, et al. Clinical approach to anterior adhesive restorations using resin composite veneers. Eur J Esthet Dent. 2007;2(2):188-209.
37. Magne P, Douglas WH. Additive contour of porcelain veneers: a key element in enamel preservation, adhesion, and esthetics for aging dentition. J Adhes Dent. 1999;1(1):81-92.
38. Ferrari M, Patroni S, Balleri P. Measurement of enamel thickness in relation to reduction for etched laminate veneers. Int J Periodontics Restorative Dent. 1992;12(5):407-413.
39. Garber DA. Rational tooth preparation for porcelain veneers. Compendium. 1991;12(5):316-320.
40. Kois JC, McGowan S. Diagnostically generated anterior tooth preparation for adhesively retained porcelain restorations: rationale and technique. J Calif Dent Assoc. 2004;32(2):161-166.
41. Friedman MJ. Porcelain veneer restorations: a clinician’s opinion about a disturbing trend. J Esthet Restor Dent. 2001;13(5):318-327.
42. Garber DA. Porcelain laminate veneers: ten years later. Part I: Tooth preparation. J Esthet Dent. 1993;5(2):56-62.
43. Castelnuovo J, Tjan AH, Phillips K, et al. Fracture load and mode of failure of ceramic veneers with different preparations. J Prosthet Dent. 2000;83(2):171-180.
44. Brunton PA, Aminian A, Wilson NH. Tooth preparation techniques for porcelain laminate veneers. Br Dent J. 2000;189(5):260-262.
45. Cherukara GP, Davis GR, Seymour KG, et al. Dentin exposure in tooth preparations for porcelain veneers: a pilot study. J Prosthet Dent. 2005;94(5):414-420.
46. Magne P, Magne M. Use of additive waxup and direct intraoral mock-up for enamel preservation with porcelain laminate veneers. Eur J Esthet Dent. 2006;1(1):10-19.
47. Gürel G. Porcelain laminate veneers: minimal tooth preparation by design. Dent Clin North Am. 2007;51(2):419-431.
48. Magne P, Belser UC. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Restor Dent. 2004;16(1):7-18.
49. Gürel G. Predictable, precise, and repeatable tooth preparation for porcelain laminate veneers. Pract Proced Aesthet Dent. 2003;15(1):17-26.
50. Merriam-Webster. Merriam-Webster’s Collegiate Dictionary, 11th Edition. 2008. Merriam-Webster.
51. Calamia JR, Calamia CS. Porcelain laminate veneers: reasons for 25 years of success. Dent Clin North Am. 2007;51(2):399-417.
52. Brunton PA, Wilson NH. Preparations for porcelain laminate veneers in general dental practice. Br Dent J. 1998;184(11):553-556.
53. Rouse JS. Full veneer versus traditional veneer preparation: a discussion of interproximal extension. J Prosthet Dent. 1997;78(6):545-549.
54. Chun YH, Raffelt C, Pfeiffer H, et al. Restoring strength of incisors with veneers and full ceramic crowns. J Adhes Dent. 2010;12(1):45-54.
55. Stappert CF, Ozden U, Att W, et al. Marginal accuracy of press-ceramic veneers influenced by preparation design and fatigue. Am J Dent. 2007;20(6):380-384.
56. Magne P, Douglas WH. Cumulative effects of successive restorative procedures on anterior crown flexure: intact versus veneered incisors. Quintessence Int. 2000;31(1):5-18.