You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
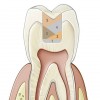
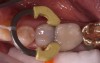
The most common problems associated with direct composite restorations include the time- and labor-intensive nature of the layering techniques involved with their placement, issues surrounding material adaptation, difficulty achieving tight contacts, polymerization and volumetric shrinkage, postoperative sensitivity, and microleakage leading to secondary caries.1,2 Composite layering protocol is dependent on restoration depth. Contributing to the time-intensive and technique-sensitive nature of multiple-layer restorations are the challenges encountered when ensuring that all composite layers combine properly and adapt well to each other and cavity walls, without producing porosities and voids (Figure 1).3
The reason composites must be layered and adapted to each other and cavity walls is to reduce the shrinkage stress produced during polymerization due to a restoration’s shape (ie, configuration [C]-factor). This C-factor, which is defined as the ratio of the restoration’s bonded to unbonded (ie, free) surfaces, influences the integrity of the composite/adhesive bonding to dentin. The fewer surfaces that are engaged by a composite increment at one time (eg, two surfaces), the lower the C-factor, the greater the bond strength, and the lower the amount of shrinkage stress there will be.4,5
Therefore, carefully adapting composite material to tooth structure and previously placed composite layers is significant to restorative success. Unfortunately, although layering multiple composite increments into the preparation design produces the least amount of stresses inside the tooth, such increments do stress the various bond strengths of the previously placed layers.6 Additionally, any available resin typically undergoes polymerization and volumetric shrinkage, and an inherent sequela from shrinkage and improper layering and adaptation is postoperative sensitivity.2,6,7
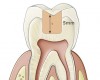
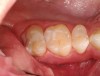
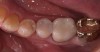
Ideally an absence of postoperative sensitivity will be long lasting, but immediately preventing postoperative sensitivity does not preclude the future occurrence of microleakage. With resin-based materials, microleakage is inevitable over time due to material breakdown and failure from wear and various intraoral proteases.1,2 The No. 1 reason for composite failure is recurrent decay, and the floor of the proximal box of a Class II restoration is the most vulnerable area (Figure 2).1,2
To help maintain marginal integrity and prevent microleakage, a low-stress composite adaptation is required at this most vulnerable area, and every attempt should be made to ensure minimal shrinkage stress.2,8 Additionally, particularly for Class II restorations, creating tight contacts is essential and requires well-adapted materials that are tightly and sufficiently packed to ensure good contacts and an ideal emergence angle.2,7 Contacts should be broad throughout the range of tooth structure because it touches the opposing tooth.
Bulk-fill Composites
To resolve problems associated with direct composite restorations, manufacturers have introduced products with greater user-friendly handling characteristics that are faster and easier to use and that minimize the amount of polymerization and volumetric shrinkage that occurs in direct composites.9-12 These have included bulk-fill composite materials, which were originally introduced in the 1990s. Since then, ongoing advancements and developments within this composite category have demonstrated further improvements in some properties compared with earlier generations of bulk-fill resins, but challenges remain with volumetric shrinkage and stress. Research has shown that volumetric shrinkage and stress of bulk-fill composites are not necessarily less than other conventional restorative resins but could be no more than equivalent.13
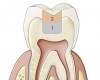
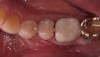
Bulk-fill composite materials are available today that can be placed in increments up to 4 mm or more (Figure 3), which is advantageous compared with 2-mm layering techniques, and cured in 10-second increments. For a shallow cavity up to 4-mm deep, light-cured dentin and enamel replacement bulk-fill composites can be placed in a single increment to replace both dentin and enamel.
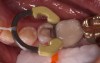
However, when preparation depths approach 6 mm, the use of two increments (eg, a dentin replacement layer deep in the preparation that is topped with a modern composite) has been advocated.14 Light-cured flowable bulk-fill dentin replacement composites have been used the longest. These materials are placed as the first increment to replace the dentin, after which modern composite is placed on top. Typically demonstrating volumetric shrinkage between 3% and 6%, as well as relatively low shrinkage stresses between 1.6 MPa and 3 MPa, they have worked well when proper adhesive bonding techniques are followed. This technique is preferred when preparations are deeper than 4 mm (Figure 4 through Figure 12).
Recent published research has indicated that marginal adaptation similar to conventional multi-layer techniques can be achieved more quickly using a bulk-fill composite.10 This suggests that using a bulk-fill composite can potentially deliver the same type of result as incremental layering and/or incremental bulk-fill layering, without the problems associated with layer adaptation, time intensity, or microleakage. Other research has concluded that using a bulk-fill composite restorative material results in a similar proportion of gap-free tooth restoration interfaces to the use of conventional composite.11 However, this again is dependent on technique proficiency and the defect being restored.
Dual-Cured Bulk-fill Materials
Manufacturers have begun introducing nano-filled, low viscosity dual-cured bulk-fill composites that demonstrate a slower rate of self-curing to reduce stresses at the bonded interface.12,14,15 Slower polymerization and shrinkage could, in theory, produce lower stresses at the tooth interface and decreased marginal gap formation.12
This type of bulk-fill composite eliminates the need for flowable liners and incremental curing, yet its viscosity enables good adaptation to preparation walls. It self-cures after placement within 2 to 4 minutes, but an additional 30-second light-cure can be performed after it is done self-curing but prior to finishing (Figure 13 through Figure 16).
Because curing lights cannot always penetrate to the bottom of deeper preparations (eg, 8 mm), or the curing light may not be correct for the material used, dual-cured bulk-filled composites for replacing both enamel and dentin can be particularly beneficial. Clinicians can place the material in bulk from bottom to top in large defects, and the materials will self-cure to any depth possible with lower stress.12,14,15 However, achieving optimal bond strengths is predicated on using an adhesive bonding agent compatible with dual-cure resins.16
Conclusion
The concept of bulk-filling restorations demonstrates great promise and has the potential to perform well in many situations. Although more research and further material improvements are needed, bulk-fill composites are the fastest-growing category in dentistry due to the convenient and time-saving techniques that can be used for their placement. Overall, however, the technique(s) employed for their placement remain the most critical components for evaluation. Clinicians must determine for themselves what the risks and longevity are for their technique and materials.
References
1. Christensen GJ. Remaining challenges with class II resin-based composite restorations. J Am Dent Assoc. 2007;138(11): 1487-1489.
2. Fabianelli A, Sgarra A, Goracci C, et al. Microleakage in class II restorations: open vs closed centripetal build-up technique. Oper Dent. 2010;35(3):308-313.
3. Souza-Junior EJ, de Souza-Régis MR, Alonso RC, et al. Effect of the curing method and composite volume on marginal and internal adaptation of composite restoratives. Oper Dent. 2011;36(2):231-238.
4. Feilzer AJ, De Gee AJ, Davidson CL. Setting stress in composite resin in relation to configuration of the restoration. J Dent Res. 1987;66(11):1636-1639.
5. Nikolaenko SA, Lohbauer U, Roggendorf M, et al. Influence of c-factor and layering technique on microtensile bond strength to dentin. Dent Mater. 2004;20(6):579-585.
6. Van Meerbeek B, Peumans M, Poitevin A, et al. Relationship between bond-strength tests and clinical outcomes. Dent Mater. 2010;26(2):e100-e121.
7. Ruiz JL, Mitra S. Using cavity liners with direct posterior composite restorations. Compend Contin Educ Dent. 2006;27(6):347-351.
8. Rodrigues Junior SA, Pin LF, Machado G, et al. Influence of different restorative techniques on marginal seal of class II composite restorations. J Appl Oral Sci. 2010;18(1):37-43.
9. Van Ende A, De Munck J, Mine A, et al. Does a low-shrinking composite induce less stress at the adhesive interface? Dent Mater. 2010;26(3):215-222.
10. Campos EA, Ardu S, Lefever D, et al. Marginal adaptation of class II cavities restored with bulk-fill composites. J Dent. 2014;42(5):575-581.
11. Furness A, Tadros MY, Looney SW, Rueggeberg FA. Effect of bulk/incremental fill on internal gap formation of bulk-fill composites. J Dent. 2014;42(4):439-449.
12. Vandewalker JP, Casey JA, Lincoln TA, Vandewalle KS. Properties of dual-cure, bulk-fill composite resin restorative materials. Gen Dent. 2016:64(2):68-73.
13. Algamaiah H, Sampaio CS, Rigo LC, et al. Microcomputed tomography evaluation of volumetric shrinkage of bulk-fill composites in class II cavities. J Esthet Restor Dent. 2017;29(2):118-127.
14. Van Ende A, De Munck J, Lise DP, Van Meerbeek B. Bulk-fill composites: a review of the current literature. J Adhes Dent. 2017;19(2):95-109.
15. Jung JH, Park SH. Comparison of polymerization shrinkage, physical properties, and marginal adaptation of flowable and restorative bulk fill resin-based composites. Oper Dent. 2017;42(4):375-386.
16. Crim GA. Influence of bonding agents and composites on microleakage. J Prosthet Dent. 1989;61(5):571-574.