You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
For many dentists, the production and placement of crowns is the lifeblood of their practice, often accounting for a large portion of the business. Nationally, the average practice places around 13 single-unit crowns per month, or just over 150 per year.1 The transfer of accurate records to the dental laboratory is a vital part of the fabrication of crowns and bridges. Obtaining optimal gingival displacement and ideal impressions is one of the most challenging procedures in dentistry. Clinicians must be able to identify and analyze the quality of their impressions, which will ultimately determine the success of their restorations.
Many studies have been conducted evaluating the quality of impressions. In 2005, one such study showed that 89% of all impressions had at least one appreciable error.2 If impression materials are constantly improving, why aren't the impressions getting better? The answer lies in the handling of impression material, proper selection of impression trays, and techniques used in soft-tissue displacement.
Managing Gingival Tissues
Managing gingival tissues for impressioning has many challenges. Though an impression may appear fine when taken, often the clinician will notice that the final version has some deficiencies, such as continuing bleeding points, tissue overlap, and/or many small imperfections. Having to take multiple preparations can further exacerbate the problem, while digital scanning requires even greater skill and finesse. Clinicians can learn to appreciate the value of dental laboratory technicians by communicating with them to troubleshoot impressions and preparations. Through proactive communication with their laboratory technicians, clinicians can overcome many of the drawbacks of impression-taking.
Technicians can relay information to clinicians about errors they encounter daily. The aforementioned survey showed that 50.7% of impressions had voids or tears at the finish line, 44% had putty impression material showing through the wash, and 40.4% had air bubbles at the finish line, to name some of the types of errors encountered.2 A recent article in the Journal of the American Dental Association (JADA) showcased a similar breakdown of errors, noting that marginal discrepancies made up the largest category of errors observed in impressions evaluated.3 These statistics illustrate the importance of clinicians providing dental technicians impressions that are readable and usable and that will enable the production of final crowns that are clinically exceptional.
Tissue Retraction
Tissue retraction is the key to obtaining superb impressions because soft tissue must be out of the way of the preparation margin. Retraction is the downward and outward movement of the free gingival margin. The gingiva needs to be displaced so a clear view of the finish line of the prepared tooth can be attained. Once this is accomplished, space is made available for the impression material to flow and for details to be recorded. Essentially, the gingival retraction material must create a trough free of blood and fluids and do so without causing any damage to the gingiva.4
A gingival retraction material must meet three criteria to be considered effectual.5,6 First, the material should be effective in both performing gingival retraction and, if necessary, achieving hemostasis. Most likely, unless the clinician is looking to restore only supragingivally, some bleeding will occur, and there must be a measure in place to stop it. Second, the material should cause no systemic effects, eg, the patient's heart rate should not become elevated as a result of using the material. Third and most importantly, use of the material should cause no irreversible damage to gingival tissues.5,6
Many different gingival retraction materials have been used over the years. Still, often when a patient returns for final cementation of the crown, damage to the tissue is evident. Sometimes the tissue may have shrunk and exposed the margin, which can be highly problematic if it has occurred in the anterior. Thus, it is crucial to understand how gingival retraction can be successfully implemented to avoid tissue damage. Gingival retraction can be achieved in five different ways: mechanical, chemo-mechanical, surgical, retraction paste, and any combination of these methods.6-8
Mechanical Retraction
To perform mechanical retraction, one of three methods can be followed: placement of a rubber dam, a technique that does not seem to be used much today; use of a copper band, a once-popular method that is considered primarily a thing of the past; and use of cotton retraction cord, the most prevalent method used today. Retraction cord is either plain, twisted, braided, or knotted, and it can be single- or double-stranded. It is available in many shapes; sizes include 000 (thinnest), 00, 0, 1, 2, and 3 (thickest). The cord also can be impregnated with different chemicals. Epinephrine is sometimes placed within the cord.6-8 The smaller cord sizes are used primarily in a double-cord technique, in which the clinician places a small cord in the trough first and then a larger cord on top of it.7,8Placing retraction cords successfully can be a time-consuming process, taking up to 5 minutes or more.7,8 Figure 1 depicts a diagram of a cord in place, where the tooth has been prepared and a retraction cord has been placed to drive the gingiva out of the way.
Placing cord requires appropriate force. Placing retraction cord requires slightly more pressure than when probing; however, too much pressure may damage the epithelial attachment.
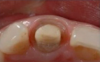
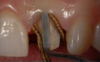
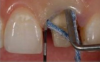
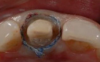
An advantage of using cord technique is that it generally provides an accurate and precise measurement,7,8 physically separating the gingiva away from the prepared margin to allow the clinician to insert light-body material to flow below the margin. Additionally, if a double-cord technique is used, the clinician can leave the bottom cord in place. Moreover, no new equipment is required, and chemicals may not be needed. The clinician needs only the cord and a cord packing instrument. Drawbacks to using cord are the risk of epithelial attachment injury, some pain that may necessitate the use of local anesthesia, a level of technique sensitivity that typically requires practice on the part of the clinician to become skilled, the likelihood of bleeding, and the risk of irreversible gingival injury that may lead to permanent recession.9,10 Figure 2 through Figure 5 show close-up photographs of a prepared tooth and margin, cord being packed, cord in place, and margin after cord removal, respectively.
Chemo-Mechanical Retraction
Chemo-mechanical retraction combines the chemical action of different materials with pressure from the packing cord. This involves cord being dipped into a solution. Historically, one of the most common solutions is zinc chloride. Other solutions that were common in the past included sulfuric acid and trichloroacetic acid. The most commonly used chemicals today are hemostatic astringents, such as aluminum chloride, aluminum sulfate, and ferric sulfate, and the vasoconstrictor epinephrine. The cord can be dipped into one of these chemical solutions to moisten it, and then packed to create hemostasis.11-13
Care must be taken when using epinephrine materials because they have systemic effects such as tachycardia, rapid respiration, elevated blood pressure, and anxiety.14-16 Epinephrine should be utilized judiciously and should not be used with patients who have high blood pressure, cardiovascular disease, diabetes, or hyperthyroidism or with patients who are taking medications such as beta blockers.14-16
Surgical Retraction
Surgical retraction techniques can be used to open up the gingival area for the placement of material. There are three surgical methods: gingival curettage, electrosurgery, and laser retraction. Gingival curettage refers to the use of a crown preparation diamond to create a trough along the margin. This removes some of the epithelial tissue in the sulcus as the clinician simultaneously finishes the preparation. Commonly, when preparing a tooth, the clinician extends subgingivally in the anterior area to hide the margin or goes below the existing restoration subgingivally in the posterior area. As the clinician performs the preparation, the diamond is often wide enough to remove a small portion of the epithelial lining of the sulcus and create a good trough. This enables clear visualization of the preparation without the use of cord.
Electrosurgery, which in essence cuts tissue with an electrode, uses a high-frequency oscillator or radio transmitter that delivers a high-frequency electrical current. This achieves controlled tissue destruction via the current flowing through a small cutting electrode that produces high current density and rapid temperature rise. The electrode, which is extremely skinny, almost needle-like, is moved around the bottom edge of the preparation to create a trough.
Advantages to the use of electrosurgery when performed properly are that a clear opening is created with no bleeding, healing occurs by primary intention, only slight pressure is needed to incise the tissue, and there is minimal tissue loss after healing.17-20 A disadvantage of electrosurgery is an unpleasant odor that can result from the melting of tissue, which can potentially cause anxiety for the patient. Also, if done incorrectly, it can lead to crestal bone loss.19,20Another drawback of electrosurgery is that it cannot be used on thin tissue.19,20
The third method of surgical retraction in the sulcus for obtaining a good impression is the use of a laser. Both diode and neodymium-doped yttrium aluminum garnet (Nd:YAG) lasers create hemostasis with minimal tissue removal, and typically the tissue heals nicely.10,21 Often an anesthetic is not needed when using a soft-tissue laser because discomfort to the patient is minimal. However, as with electrosurgery, an unpleasant odor may occur from the melting of tissue.
Retraction Paste
The use of retraction paste (eg: DryZ®, Parkell, parkell.com; Expasyl™, Kerr Dental, kerrdental.com; Traxodent™, Premier Dental, premusa.com) is a method favored for its many advantages. The body of the paste typically is composed of kaolin, clay, and aluminum chloride for hemostasis. The author finds that to achieve optimal results, retraction caps should be used. Advantages of using retraction paste are that it effectively achieves hemostasis due to the incorporation of aluminum chloride, it absorbs crevicular fluid so that the crevice is dry after rinsing, it is atraumatic, no tissue discoloration occurs, and it is easy to dispense and rinse off.6,22 Additionally, it is less time-consuming than other methods, requiring only the dispensing of the paste, inserting the retraction cap, and having the patient bite down.
Retraction paste also can be used in other clinical situations, such as placing composites and cementing crowns.6,7 For example, when performing an anterior Class V composite restoration where the gums might be prone to bleed, the clinician can apply the paste and allow hemostasis to take place before placing the composite material.
Disadvantages to using paste can stem from not getting tissue as dry as possible before placement.22 If the tissue is already bleeding, the clinician should apply pressure to dry the tissue before placing the paste. Also, sometimes the tip of the dispensing unit may be too large for the particular application and the paste will not flow down deep into the sulcus unless a retraction cap is used to physically push the tip in.22 Additionally, the use of paste typically is slightly more expensive compared with other methods.22 Using unit-dose syringes can make it easier to deliver an exact amount of paste, although they are an additional expense.
Finally, the author recommends using retraction caps (eg, ROEKO Comprecap®, Coltene, coltene.com; Premier® Retraction Caps, Premier Dental, premusa.com; GingiCap™, Centrix, centrixdental.com) when paste is used to achieve gingival retraction. These cotton-based caps offer moisture absorption and provide patients a comfortable means of resting their bite after having remained open for long periods of time. Most importantly, the compression force onto the retraction paste helps with hemostasis.23
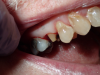
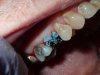
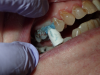
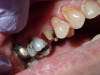
Figure 6 through Figure 9 demonstrate the use of retraction paste and a cap. An upper bicuspid was prepared (Figure 6), and some bleeding occurred due to the clinician working below the existing restorations. Retraction paste was then applied (Figure 7), but there was still some residual bleeding. The clinician then had the patient close on the retraction cap to stop the bleeding (Figure 8). Some blanching occurred as the patient bit into the cap. The patient will hold that position depending on how much bleeding occurs. Figure 9 shows the exposed margin ready for impressioning. In this case, the retraction cap was kept in place with the patient biting down on it for 2 to 3 minutes instead of 1 to 2 minutes because there was a fair amount of bleeding initially.
Figure 10 through Figure 12 are examples of final impressions taken with retraction paste alone. No cord or soft-tissue diode laser was used. Figure 10 shows an impression on which the clinician went quite far subgingivally and achieved a clean margin, including an excavated area on the labial surface. These examples demonstrate how consistent the use of retraction paste can be.
Combination of Methods
Any of the methods previously mentioned can be used together to gain maximum hemostasis and tissue retraction.7 An example of a combination method is to pack cord first, then place retraction paste and use a cap. Alternately, a diode laser could be used before the cord and retraction paste are placed. Whatever method or combination of methods is chosen, the end goal is to achieve an excellent impression that results in a superb final restoration.
Technology has created a new armamentarium for clinicians. Scanning, for example, is used more frequently now for crowns and bridgework. It requires meticulous, clean, and dry retraction because a crown cannot be designed on a computer screen unless the clinician can see the margins perfectly. Also, the laboratory cannot work on a scan unless there is a clean margin.
Conclusion
Success in impression-taking lies in the details and not rushing the process. The final restoration is only as good as the impression. Crowns and bridgework depend significantly on effective management of gingival tissue through tissue retraction techniques. Clinicians can benefit from extensive practice and trying out many different brands to determine their preferences. Tissue retraction methods can be mechanical, chemo-mechanical, surgical, paste, or any combination of all four. Each of these methods has advantages and disadvantages that may make one more suitable for different patients and clinicians, depending on their preference. Expertise in tissue retraction will lead to restorations that seat easier and have fewer adjustments. The entire process is streamlined when clinicians provide the laboratory a clean, impeccable impression.
About the Author
Jeffrey B. Dalin, DDS
Private Practice
St. Louis, Missouri
References
1. Henry K. Here's the average number of single crowns dentists are placing (and where the trend is headed). Dentistry IQ. http://www.dentistryiq.com/articles/apex360/2017/07/here-s-the-average-number-of-single-crowns-dentists-are-placing-and-where-the-trend-is-going.html. Published July 11, 2017. Accessed December 23, 2017.
2. Samet N, Shohat M, Livny A. Weiss EI. A clinical evaluation of fixed partial denture impressions. J Prosthet Dent. 2005;94(2):112-117.
3. Rau CT, Olafsson VG, Delgado AJ, et al. The quality of fixed prosthodontics impressions: An assessment of crown and bridge impressions received at commercial laboratories. J Am Dent Assoc. 2017;148(9):654-660.
4. Lyajam S, Prasanth V. Gingival retraction techniques - a prerequisite in fixed prosthodontics: a review. Health Sciences. 2012;1(3). http://healthsciences.ac.in/oct-dec-12/Gingival-Retraction-Techniques.html. Accessed December 23, 2017.
5. Safari S, Vossoghi Sheshkalani Ma, Vossoghi Sheshkalani Mi, et al. Gingival retraction methods for fabrication of fixed partial denture: literature review. J Dent Biomater. 2016;3(2):205-213.
6. Poss S. Minimally invasive tissue management for restorative procedures. Dental CE Digest. https://www.dentalacademyofce.com/courses/1462/pdf/minimallyinvasivetissuemgmt.pdf. Accessed December 23, 2017.
7. Strassler HE, Boksman L. Tissue management, gingival retraction and hemostasis. Oral Health. https://www.oralhealthgroup.com/features/tissue-management-gingival-retraction-and-hemostasis/. Published July 1, 2011. Accessed December 23, 2017.
8. Brinker SP. Advances in retraction. Dentistry IQ. http://www.dentistryiq.com/articles/2012/06/advances-in-retraction-dad-june2012.html. Published June 22, 2012. Accessed December 23, 2017.
9. Prasad KD, Hegde C, Agrawal G, Shetty M. Gingival displacement in prosthodontics: a critical review of existing methods. J Interdiscip Dentistry. 2011;1(2):80-86.
10. Scott A. Use of an erbium laser in lieu of retraction cord: a modern technique. Gen Dent. 2005;53(2):116-119.
11. Rosenstiel SF. Tissue management and impression making. In: Rosensteil SF, Land MF, Fujimoto J, eds. Contemporary Fixed Prosthodontics. 4th ed. St. Louis, MO: Mosby-Elsevier; 2006:431-465.
12. Morgano SM, Malone WF, Gregoire SE, Goldenberg BS. Tissue management with dental impression materials. Am J Dent. 1989;2(5):279-284.
13. Benson BW, Bomberg TJ, Hatch RA, Hoffman, Jr W. Tissue displacement methods in fixed prosthodontics. J Prosthet Dent. 1986;55(2):175-181.
14. Hansen PA, Tira DE, Barlow J. Current methods of finish-line exposure by practicing prosthodontists. J Prosthodont. 1999;8(3):163-170.
15. Fazekas A, Caempesz F, Csabai Z, Vag J. Effects of pre-soaked retraction cords on the microcirculation of the human gingival margin. Oper Dent. 2002;27(4):343-348.
16. Bader JD, Bonito AJ, Shugars DA. A systematic review of cardiovascular effects of epinephrine on hypertensive dental patients. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2002;93(6):647-753.
17. DeVitre R, Galburt RB, Maness WJ. Biometric comparison of bur and electrosurgical retraction methods. J Prosthet Dent. 1985;53(2):170-182.
18. Coelho DH, Cavallars J, Rothschild EA. Gingival recession with electrosurgery for impression making. J Prosthet Dent. 1975;33(4):422-426.
19. Bashetty K, Nadig G, Kapoor S. Electrosurgery in aesthetic and restorative dentistry: a literature review and case reports. J Conserv Dent. 2009;12(4):139-144.
20. Lowe RA. Electrosurgery in esthetic/restorative practice: everyday procedures that help create excellence in dentistry. CDEWorld. https://cdeworld.com/courses/20498-Electrosurgery_in_the_Esthetic-Restorative_Practice:Everyday_Procedures_That_Help_Create_Excellence_in_Dentistry. Published June 2016. Accessed December 23, 2017.
21. Chartrand A. Integrating laser dentistry into aesthetic dentistry. Oral Health. April 1, 2005:11-13.
22. Rajambigai MA, Ramesh Raja S, Joephin Soundar SI,