You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Anterior restorations can be daunting for any clinician to design, prepare, and deliver. However, by learning the appropriate steps of managing occlusion and the wealth of information available today on smile design, this challenging endeavor can become quite manageable. Regardless of how beautiful a smile appears it still needs to be functional. Patients must be able to chew food and enunciate words properly. In addition, abusive biting forces and constant bacterial onslaught make the oral cavity a harsh environment. If the biting forces are not harnessed, the patient could experience a fractured restoration or weaken the cement, allowing bacteria to penetrate underneath the restoration resulting in recurrent caries and, ultimately, necessitating replacement.1 This article will explain how to ensure long-term success for the patient by focusing on four critical aspects: the temporomandibular joints (TMJs), the position of the anterior teeth, the functional pathways of the mandible, and a stable occlusal foundation.
Temporomandibular Joints
Assessing each individual case from a global standpoint rather than taking a tooth-by-tooth approach allows the clinician to see potential pitfalls that could occur mid- or post-treatment. Thinking globally means looking beyond the teeth and considering what makes them move and function. This begins at the TMJs. Although numerous occlusal philosophies have been debated for years, the occlusal concept that this article will discuss is equal simultaneous contact of the teeth in centric relation (CR). According to the Glossary of Prosthodontics Terms, CR is defined as “the maxillomandibular relationship in which the condyles articulate with the thinnest avascular portion of their respective disks with the complex in the anterior-superior position against the shapes of the articular eminencies. This position is independent of tooth contact.”2 Okeson goes one step further, saying, “The condyles assume this position when all of the elevator muscles are activated with no occlusal interferences. Therefore, this joint position is considered to be the most musculoskeletally stable position of the mandible.”3
While the TMJs may seem like a curious place to begin treatment planning anterior restorations, the reason for this is simple: the TMJs are the first determinant of occlusion. Starting with the TMJs in CR provides a bone-braced position, allowing for a repeatable constant to return to time and time again throughout the course of treatment. If the joints are not fully seated in CR and are positioned slightly down the articular eminence, a disturbance within the neuromuscular system can occur. This is in large part a result of the occlusion not coinciding with CR but rather with a maximum intercuspation (MIP) tooth position. The elevator muscles, as well as the lateral pterygoids, have to contract in order to brace the condyle-disc assembly against the downward slope of the eminence. When this discrepancy exists the result can be orofacial pain, loose teeth, migration of teeth, or even fractured restorations.4 Therefore, when beginning to design an incisal edge made of porcelain, the first determinant of occlusion must be a bone-braced, repeatable position.
While joint position is extremely important, determining the joint condition is equally important. Key considerations include whether or not the TMJs are able to accept firm loading in CR utilizing bimanual manipulation, or whether any popping/clicking occurs within the joint assembly upon opening/closing. Also, the clinician should note if the patient displays any facial/mandibular asymmetries that could further indicate a problem. Noticing facial asymmetries or compromised growth patterns can help in spotting a possible TMJ derangement when treatment planning a case. If facial asymmetries are observed, typically the chin deviates to the side of the diseased joint. However, if a patient were to exhibit a severe class II skeletal profile, bilateral derangements may have potentially compromised the growth of the condyles, resulting in an underdeveloped mandible. Either result can lead to a loss in vertical dimension of the affected TMJs.5 When a possible derangement is suspected, a magnetic resonance image or cone-beam computed tomography should be considered for further determination prior to beginning treatment.
By paying close attention to the joint position as well as condition, the clinician can determine if any foundational issues exist within the joint that could compromise the restorations either immediately or long term. This information can also help the patient understand and take ownership of the condition rather than shift blame back to the dentist if subsequent problems were to arise.
Functional Smile Design
Once the first determinant of occlusion, TMJs, has been closely analyzed and the clinician has determined that it is safe to proceed, the next consideration in designing beautiful anterior restorations is understanding current smile design principles. While it is easy for dentists to get caught up in the fine-detail micro-esthetic principles of smile design such as surface texture, line angles, and shade, they must remain cognizant of the macro-esthetic principles of how the teeth appear in the smile and facial proportions. A smile needs to fit the macro-esthetic and micro-esthetic objectives of the patient as well as the functional requirements needed to ensure success.6 Even though certain smile design features are subjective, such as color, shade, and texture, other aspects like tooth position, phonetics, and occlusion are objective. These objective principles work conjointly with the aforementioned occlusal principles, ie, form follows function. When a clinician understands that form and function are not completely separate entities, it allows for esthetic restorations that are not only beautiful but also promote functional harmony within the neuromuscular system.7 Because each patient’s smile is unique, for each case a different set of functional parameters will dictate the form to follow. This is paramount for the clinician to recognize in order to create smiles that mimic natural esthetics.8
To begin developing a patient’s smile, the maxillary central incisors must be positioned correctly from a horizontal and vertical standpoint. Ideally, the facial midline would bisect the central incisors to allow for proper symmetry within the smile and facial proportions. Once the incisal edges of the maxillary central incisors have been set, the smile is continued posteriorly, moving to the laterals, canines, and buccal cusps of the premolars and molars.9 The upper incisal edges should follow the inner vermillion border of the lower lip to provide a gradual curve back through the buccal corridor. To ensure a smooth transition from anterior to posterior teeth, the clinician should utilize photographs that show the front and lateral smile views. These will provide a better visualization of how many teeth need to be included in the design to avoid any stark contrast between the posterior and anterior teeth.10
By using a full series of photographs and facebow-mounted casts in CR to treatment-plan the case, a wax-up can be established in very close accuracy to the needed incisal edge position. However, the final position would be fine-tuned in the provisional stage prior to fabricating the final restorations. The wax-up serves as the blueprint for both the clinician and patient to begin to envision the potential changes for the new smile design and allows for a transfer of that information to the mouth in the form of functional esthetic provisionals.11 Once the patient has approved the provisionals for esthetics, phonetics, and function, this information can be communicated to the laboratory in the form of a facebow-mounted, approved provisional cast. This then serves as a 3-dimensional representation of the new incisal edge position. When done properly and precisely, this allows the ceramist to fabricate the final restorations according to the approved provisionals, which results in minimal adjustments at the insert appointment.12
Anterior Guidance and Mandibular Movement
The concept of anterior guidance is of great importance for placing anterior restorations that can withstand the functional requirements of the oral cavity. By allowing the anterior teeth to contact simultaneously in CR along with the posterior teeth, the load of the elevator muscles can remain even and in harmony with one another. Then, once the lateral pterygoid muscle begins to contract to translate the condyle and disc assembly down the articular eminence in a laterotrusive movement, the lingual contours of anterior teeth can provide an immediate disclusion of the posterior teeth. Williamson and Lundquist proved this by using electromyographic studies to show reduced elevator muscle activity by eliminating posterior contacts in laterotrusive movements through canine and anterior guidance. However, if any posterior teeth are allowed to interfere with this movement, the elevator muscles contract.13 If this occurs, the consequences can become detrimental to the neuromusculature as well as the dentition, resulting in wear or fractured restorations.14 Dawson stated that a customized anterior guidance needs to be established for each patient based on his or her individual needs.15 Certain patients will need a steeper anterior guidance while some will require a more horizontal one; however, the anterior guidance has to be steep enough to ensure immediate posterior disclusion while remaining in harmony with the envelope of function.15
Two main concepts apply regarding proper anterior teeth interaction during the functional pathways of the mandible. First is the envelope of motion, which is the outer limit of the mandibular movements. The envelope of motion is dictated by the TMJs and supporting structures such as ligaments, bones, and muscles. The second concept is the envelope of function, which is the mandibular movement within the confines of the envelope of motion.16 During these movements the lower lip must function effortlessly in relation to the maxillary incisal edges to ensure proper phonetics and utility. If the edge is too far facially then the “s,” “v,” and “f” sounds could be difficult for the patient to articulate. This could also result in a lack of anterior guidance and excessive muscle hyperactivity from the posterior teeth, interfering with the laterotrusive movements of the mandible. Conversely, if the teeth are too far lingually or if the teeth need to have length added, this could interfere with the envelope of function causing a disturbance to the neuromusculature and potentially leading to wear of the opposing teeth or fracture of the new restorations. This further reiterates the reasoning for starting with mounted casts in CR to closely analyze the occlusion prior to beginning treatment.17,18 Once the provisionals are placed, the patient’s functional pathways can be monitored to ensure proper esthetics, phonetics, and function.
One final key item to check when restoring anterior teeth is long centric. Long centric provides horizontal freedom for the anterior teeth when bodily postural change occurs from the supine position to the upright position. This allows for a slight horizontal movement of the mandible from CR so as to not interfere with the closure path of the mandible with the anterior teeth. The movement in long centric results in the condyles moving down the eminence slightly from CR in a protrusive manner.19 This relates back to the functional pathways of the mandible and treating it from inside to outside movement. By treating the patient inside-out, it reduces that chance of posterior teeth interfering with chewing. Even though a chewing stroke is an outside to inside movement, if the patient has a proper anterior guidance that does not interfere with the envelope of function and the room that may be needed for long centric, the posterior teeth should not interfere in any of the functional pathways even at the outer edge of the envelope of motion.
Occlusal Scheme
When analyzing the occlusion in the mouth and on mounted casts, clinicians must decide whether to restore patients in their current habitual occlusion (ie, MIP) or reposition the mandible to CR and allow the teeth contact to coincide with that position. The clinician must bear in mind that occlusion is not static; it is a functional relationship that can result in malocclusions, muscular dysfunction, and bruxing of teeth.20 If any signs or symptoms of instability exist within the current occlusion prior to starting treatment, a plan needs to be designed that will create a more favorable environment for the restorations. By placing restorations into the same unstable environment with nothing being changed, clinicians cannot expect the restorations, made of porcelain, to hold up any better than the natural teeth, made of enamel and dentin.
There are multiple ways to alter occlusion to allow for a more harmonious result, but the end-goal remains the same: to create a more positive environment to prevent further breakdown of the TMJs, dentition, restorations, or supporting structures. A stable occlusion starts with the condyle disc assembly in CR and simultaneous tooth contact between the maxillary and mandibular teeth. The posterior teeth should not interfere with the movement of the mandible from CR. Additionally, the anterior guidance should be developed within the envelope of function.21 The most simple and conservative way to accomplish this stable relationship is to eliminate the discrepancy between CR and MIP by occlusal equilibration. Ideally, this would be initiated before any fixed prosthodontics work is completed.22 However, equilibration can often be incorporated during the prepping and provisionalization phases of treatment.
Case Example
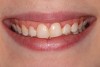
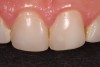
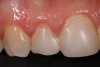
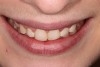
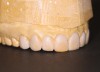
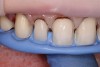
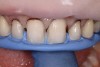
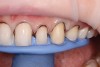
The following case example demonstrates this restorative approach. A young female patient presented to the office with composite veneers on teeth Nos. 7 through 11. She was uphappy with the shape, size, color, and contours of the composites (Figure 1 and Figure 2). Her other primary complaint was that the composites were in constant disrepair. There were multiple patches used in attempts to repair the composite veneers (Figure 3), but that strategy was proving to be very frustrating to the patient rather than a convenience. The patient was now motivated to have a beautiful smile she could be proud of and not constantly have to fix or repair.
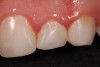
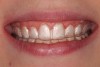
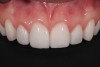
The patient was evaluated with a complete examination that included a full set of photographs, periodontal probings, and facebow-mounted casts in CR. From this information, it was evident that the patient displayed a significant 3-mm slide from CR to MIP. Using Doppler auscultation it was determined that there was a left lateral pole recapture or “click” upon opening and translation down the articular eminence. The patient was able to accept firm loading in CR using bimanual manipulation. This discrepancy was believed to have caused a traumatic occlusion on the anterior composites, resulting in the constant chipping. Also, the gingiva displayed localized moderate gingivitis in the upper anterior region as a result of the poorly polished composites (Figure 4 and Figure 5).
The treatment plan consisted of crown-lengthening surgery to correct the gingival levels, whitening for a lighter shade, and an equilibration prior to preparing porcelain veneers Nos. 5 through 12 to stabilize the occlusion. The working position would be CR to ensure a more positive occlusal environment moving forward.
The incisal edge position of tooth No. 8 was determined to be closest to ideal, so it was used as a reference point (Figure 6). A surgical guide was fabricated from the wax-up for the periodontist to complete the crown lengthening (Figure 7 and Figure 8). This can be made using an acrylic mock-up or a clear suck-down. The guide can then be transferred to the patient’s mouth to allow for predictable gingival margin placement (Figure 9).23
Once the crown-lengthening surgery was completed the patient was allowed sufficient time to heal, professional whitening (35% Opalescence®, Ultradent Products, Inc., www.ultradent.com) was used in customized professional take-home whitening trays. The patient reached a shade of B1 and was ready to proceed with the restorations. She was equilibrated to provide stable centric stops and anterior/canine guidance and prepped for veneers Nos. 5 through 12 using preparation guides from the wax-up (Figure 10 through Figure 12).
After the functional esthetic provisionals were placed, the focus was on attaining the ideal incisal edge position to satisfy the esthetic and functional aspects for the patient’s smile (Figure 13). The position was achieved and then communicated to the laboratory using a facebow-mounted, approved provisional cast. The ceramist was then able to construct a custom incisal guide table along with a 3D putty matrix for the incisal edge position. The custom incisal guide table also served as the confines within which the ceramist would work in order to achieve proper position and to not encroach upon the patient’s envelope of function.
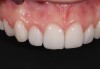
The final restorations (IPS e.max®, Ivoclar Vivadent, www.ivoclarvivadent.com) displayed a natural, lifelike appearance (Figure 14 through Figure 16). With the incisal edge in the proper horizontal and vertical position, the patient now had a smile that was effortless (Figure 17). Initially hesitant and shy (Figure 18), she now was able to boldly smile with confidence (Figure 19). Additionally, because the treatment addressed the four key concepts of the temporomandibular joints, correct position of the anterior teeth, functional pathways of the mandible, and sound occlusal foundation, the patient no longer has to worry about constantly patching her front teeth.
Conclusion
The advancements of dental materials have been amazing. Restorative materials such as zirconia and lithium disilicate are becoming increasingly popular options because of their strength, minimal reduction requirements, and esthetics. However, for patients who present to the dental office with obvious signs of occlusal instability such as worn or broken teeth, abnormal mobility, and/or fremitus,24 the solution to their problem is not simply a stronger material. The occlusal environment must be considered before proceeding. Even though new zirconia is extremely strong, something has to give in order to compensate for the hardness of the crown. As a result, the tooth moves out of position and creates an open contact, or worse, a root fracture under the stress from the occlusion. In such instances, the appropriate response is to create a stable occlusion rather than merely using a stronger material.
Ignoring the functional pathways that are associated with mandibular movement and proper tooth positioning prior to placing anterior restorations is not in the best interest of the patient. Whether it will be the restorations or the supporting structures, some aspect will likely begin to fail or break down. These issues can potentially be avoided by taking the time to analyze the TMJs, the position of the anterior teeth, the functional pathways of the mandible, and the occlusal foundation prior to preparing a case. In essence, the clinician must begin with the end in mind. When the occlusal environment is stable, beautiful esthetic restorations can be placed on anterior teeth without the concern of fracture or traumatizing effects. This, in turn, leads to satisfied patients who can proudly show their new smile and be confident that it will stand the test of time.
Questions
Queries to the authors regarding thisCE may be submitted to authorqueries@aegiscomm.com.
References
1. Kois JC. New challenges in treatment planning: incorporating the fundamentals of patient risk management. Part 2. Journal of Cosmetic Dentistry. 2011;27(1):110-123.
2. The glossary of prosthodontic terms. J Prosthet Dent. 2005;94(1):10-92.
3. Okeson JP. Criteria for optimal functional occlusion. In: Management of Temporomandibular Disorders and Occlusion. 5th ed. St. Louis, MO: Mosby; 2003:113.
4. Wilkerson DC. Critical factors of occlusion. Journal of Cosmetic Dentistry. 2012;28(3):118-124.
5. Schellhas KP, Piper MA, Bessette RW, Wilkes CH. Mandibular retrusion, temporomandibular joint derangement, and orthognathic surgery planning. Plast Reconstr Surg. 1992;90(2):218-229.
6. Morley J, Eubank J. Macroesthetic elements of smile design. J Am Dent Assoc. 2001;132(1):39-45.
7. Cobb AC. Complete treatment planning: meeting patients’ needs. Inside Dentistry. 2015;11(8):66-70.
8. Cranham J, Finlay S. Timeless principles in esthetic dentistry. Journal of Cosmetic Dentistry. 2012;28(3):60-68.
9. Spear FM, Kokich VG, Mathews DP. Interdisciplinary management of anterior dental esthetics. J Am Dent Assoc. 2006;137(2):160-169.
10. Olitsky J. Seven worst violations of smile design: achieve better esthetics by understanding common mistakes. Inside Dentistry. 2015;11(9):60-68.
11. Dudney TE. Using diagnostic wax-ups and preparation guides to facilitate accurate and esthetic diastema closure and functional bite alteration. Inside Dentistry. 2008;4(7):54-57.
12. Sesemann MR. Diagnostic full-coverage provisionals for accurately communicating esthetic and functional provisionalization. Functional Esthetics & Restorative Dentistry. 2008;2(2):8-15.
13. Williamson EH, Lundquist DO. Anterior guidance: its effects on electromyographic activity of the temporal and masseter muscles. J Prosthet Dent. 1983;49(6):816-823.
14. Cranham J. Anterior guidance: myth or mandatory? An examination of the role the anterior teeth play in occlusal stability. Inside Dentistry. 2015;11(2):94-101.
15. Dawson P. Anterior guidance and its relationship to smile design. In: Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007:159-175.
16. Dawson P. The envelope of function. In: Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007:141-147.
17. Hess LA. Management of the incisal edge: the key to functional and esthetic success in anterior restorations. Inside Dentistry. 2013;9(10):56-64.
18. LeSage B. Revisiting the design of minimal and no-preparation veneers: a step-by-step technique. J Calif Dent Assoc. 2010;38(8):561-569.
19. Dawson P. Long centric. In: Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007:189-198.
20. Ash MM, Nelson SJ. Occlusion. In: Wheeler’s Dental Anatomy, Physiology and Occlusion. 8th ed. St. Louis, MO: Elsevier; 2003:437-496.
21. Rosenstiel SF, Land MF, Fujimoto J. Principles of occlusion. In: Contemporary Fixed Prosthodontics. 4th ed. St. Louis, MO: Mosby; 2006:110-144.
22. Rosenstiel SF, Land MF, Fujimoto J. Treatment planning. In: Contemporary Fixed Prosthodontics. 4th ed. St. Louis, MO: Mosby; 2006:82-109.
23. Spear FM, Cooney JP. Restorative interrelationships. In: Newman MG, Takei HH, Klokkevold PR, Carranza FA, eds. Carranza’s Clinical Periodontology. 10th ed. St. Louis, MO: Saunders Elsevier; 2006:1050-1069.
24. McDevitt MJ, Bibb CA. Occlusal evaluation and therapy. In: Newman MG, Takei HH, Klokkevold PR, Carranza FA, eds. Carranza’s Clinical Periodontology. 10th ed. St. Louis, MO: Saunders Elsevier; 2006:845-855.
About the Author
Zachary S. Sisler, DDS
Private Practice
Shippensburg, Pennsylvania