You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Dental implants are ankylosed. They are similar and behave much like avulsed teeth that become ankylosed in their relationship to surrounding teeth after reimplantation. Infraocclusion of ankylosed teeth occurs in patients after age 20 between 25% and 60% of the time, with an average yearly infraposition rate of 0.07 mm.1 One cannot assume that teeth and implants will remain in the same occlusal relationship to each other or the opposing dentition over time.
Continued vertical growth and eruption of teeth may cause infraocclusion of implant restorations. In other words, teeth may continue to erupt, leaving the implant restorations without occlusal contacts. These potential changes require the monitoring of occlusal contacts of teeth and implants over time. This can be done with articulating paper and 8-µm thick shimstock foil. If there is a discrepancy and the implants are in infraocclusion, the teeth need to be equilibrated until the implants are in solid contact again with the opposing dentition.
Skeletal growth slows after the second decade of life but may continue in some individuals throughout life. These long-term adult growth changes appear to be random and unpredictable and can lead to implant–restorative occlusal instability and complications.2 The direction of growth is influenced by the type of jaw relationship. The short face syndrome (SFS) produces more horizontal growth, leaving implants more palatal compared to the surrounding anterior incisors. The long face syndrome (LFS) results in higher vertical growth rates, and consequently implants become more labial in relationship to the adjacent teeth.3 Therefore, it is recommended to delay implant placement until growth is complete, which can vary by up to 6 years within each gender. Changes can occur even after age 20 and 22 but to a lesser degree.4,5
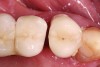
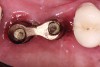
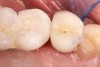
In a mixed teeth and implant dentition, horizontal growth and/or mesial drift of teeth can lead to posterior open interproximal contacts (Figure 1). The open contact can be corrected and closed by modifying the existing restoration with chairside bonding as long as the implant restoration can be easily retrieved (Figure 2). This can be accomplished in one visit (Figure 3), or porcelain can be added to the implant restoration in the laboratory. Easy, predictable retrievability is key to future serviceability of any implant restoration. Screw retention is a more predictable option than cement, as cement-retained restorations may not always be retrievable depending on the retention and the type of cement used.6
Occlusion-Related Issues
There are a number of matters to consider regarding occlusion when performing dental implant restorations. An overview of these issues, along with examples of images depicting some of these situations, is provided below.
Intrusion, Friction, and Contact Point Adjustments
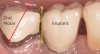
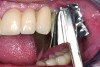
After an occlusal load is applied, the periodontal ligament (PDL) fibers return a free-standing tooth back to its original position. Teeth connected to implants with semi-precision attachments or telescoping crowns are at risk of intrusion (Figure 4). Friction prevents the natural rebounding ability of a tooth provided by the PDL fibers. In such cases, the path of draw of the attachment does not line up with all of the PDL fibers, and they, therefore, are not able to bring the tooth back into occlusion. As a result, the PDL fibers become continuously stretched. Once the tube attachment is removed and, with it, the source of friction, the tooth will become free to move on its own and will subsequently erupt spontaneously into occlusion (Figure 5). The periodontal attachment apparatus will not follow the erupting tooth, resulting in recession. Under normal circumstances a healthy attachment apparatus will move with the extruding tooth.7,8
A single tooth between two implants is vulnerable to friction as well. If the contacts are too tight the tooth cannot rebound from occlusal and horizontal forces. The PDL fibers can be stretched and the attachment apparatus damaged just like in the previous example. The contact pressure needs to be adjusted until shimstock foil can be pulled out with only slight resistance or drag (Figure 6). The adjustment is complete when the tooth is able to rebound on its own when pushed facially or lingually. The contact relationship can change and open up if the tooth were to erupt and change position in the future. A nightguard or retainer can help prevent those changes from occurring.
Occlusion on Teeth Vs. Implants
Without periodontium and periodontal mechanoreceptor feedback, fine motor control of mastication is lessened; however, this does not affect function.9,10 There is no significant difference in function between full-arch fixed prostheses on teeth in comparison to implants. Splinted teeth in a full-arch restoration have less proprioception than individual teeth, making splinted teeth more similar to implants. There, thus, may not be a significant need or benefit to retain teeth solely for the sake of improved proprioception to increase function and protect implant restorations from occlusal overload. Implants seem to develop osseoperception via a new peripheral feedback pathway, thereby establishing implant-mediated sensory-motor control.11 Retaining teeth would become of lesser importance relative to other factors in treatment planning full-arch implant restorations.
A systematic review of 1,315 studies on occlusion over a span of 40 years that examined complete dentures and reconstruction on teeth and implants found only one agreed-upon recommended occlusal design: Lingualized posterior occlusion was preferred for a complete removable prosthesis.12 All other designs have evolved from clinical experience without any scientific evidence that one design is superior.
Implants are metal objects subjected to bending forces and fatigue over long periods of time. This can lead to microcrack formation resulting in implant fractures or loosening of components.13-16 This is another reason to carefully design implant occlusion that minimizes eccentric tipping forces on implant restorations. The choice of occlusal materials’ hardness, whether it be gold, porcelain, or acrylic resin, has no significant effect on force absorption in the bone around implants.17,18
Optimum function is primarily achieved by modifying the maxillary occlusion against any opposing dentition. Because the upper teeth provide guidance in protrusive and lateral movements of the mandible, most of the adjustments should be done in the upper jaw by reducing the incisal guidance angle. An exception is lower restorations that are overcontoured and too thick labially or buccally and cause a pathway interference. This can be corrected by thinning out the labial or buccal surfaces in the lower jaw. Steeper cusp inclination and broader occlusal tables increase load concentration19 as do pathway interferences of the mandible’s envelope of motion. Reduction of lateral forces can be further improved by partial or full-arch splinting.
Cross-Arch Stabilization and Restorative Design
Splinting that goes around the arch rather than the splinting of teeth in a straight line is known as cross-arch stabilization. It is the most effective form of splinting and makes fixed restoration of teeth possible when teeth are either periodontally or structurally too compromised to be restored individually.20 Cross-arch stabilization can immobilize mobile teeth. It protects implants that are short, are embedded in poor-quality bone, or have an unfavorable implant-to-crown ratio.
With this approach the occlusal load is shared among all teeth or implants in the arch. This reduces eccentric forces on an individual implant no matter how the implant is angled or positioned relative to the occlusal surfaces. In a full-arch restoration it allows occlusal contacts to be placed where they need to be. Forces that would be of axis for an individual implant are no longer focused on one implant. Cross-arch stabilization, however, does not replace careful management of occlusal forces, including reducing the angle of incisal guidance and, thus, lateral eccentric forces.
Full-Arch Implant Restoration: One Piece or Sections?
Many factors influence treatment-planning decisions for the restoration of an entire jaw. A one-piece restoration provides cross-arch stabilization and may be kept in function even if individual implants should fail. However, this requires that more than just the minimum number of implants are placed. Placing additional implants builds in redundancy and helps long-term survival. Historically, full-arch restorations were cast in gold and had to be cut and soldered to achieve a passive fit. Today, fit is no longer an issue due to the accuracy of computer-assisted design/computer-assisted manufacture (CAD/CAM)-milled restorations, which favors this treatment modality. Long-term maintenance, however, may require the removal and repair of the entire restoration even for a chip of just a single tooth.
The benefit of cross-arch stabilization is lost when restoring an entire arch in several sections. However, with this approach it is easier to fabricate smaller sections and repair them in the future. This also allows for a mix of teeth and implants in the dentition. Long-term survival of implant restorations done in anterior and posterior sections could be in jeopardy if just one implant were to fail in the future. It could require either remaking or splinting two sections or using the remaining implants to support a full-arch restoration. Treatment planning implant restorations for the long term gives them a better chance to remain in function and to be adapted when the foundation changes.
Occlusal Stability: Selecting Restorative Materials for Full-Arch Restorations
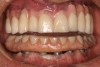
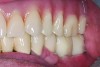
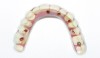
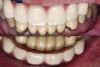
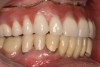
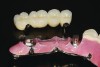
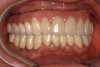
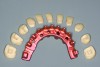
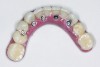
In the past, fixed full-arch implant restorations primarily consisted of gold or titanium frameworks with denture teeth processed in acrylic resin. Denture teeth are subject to wear that varies from patient to patient. Patients need to be informed that these denture teeth must be replaced on average every 8 years with a range from 5 to 12 years depending on occlusal habits and the opposing dentition.21 Heavy bruxers may wear out denture teeth faster (Figure 7 and Figure 8). Posterior denture teeth can wear faster than anterior teeth depending on the occlusal relationship between upper and lower front teeth and the type of restorative material in the opposing jaw. The resulting lack of posterior contact puts excessive force on the anterior teeth, especially in a Class I relationship, resulting in fracture or loss of upper front denture teeth. This type of occlusion requires constant supervision and adjustments. Creating a different set-up with a slight overjet taking the lower front teeth out of occlusion allows the mandible to glide from maximum posterior contact into simultaneous full anterior and posterior contact (Figure 9 through Figure 12). It is preferable to have restorative material in both jaws with similar wear characteristics. Additional choices include porcelain-fused-to-metal (PFM), lithium disilicate (eg, e.max®), and zirconia.
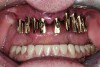
The benefits of cross-arch stabilization have been described above. The drawback of any one-piece design is the difficulty in repairing any such restoration. This can be avoided by having a full-arch framework that supports removable screw-retained PFM segments (Figure 13 and Figure 14) or individually CAD/CAM-milled cemented crowns (Figure 15 through Figure 18). This combines the strengths of a one-piece restoration with easier maintenance.
Conclusion
It is important to realize that the occlusal and contact relationship between implants and teeth may not be stable or predictable. Skeletal growth can continue in some patients throughout life to varying degrees. This can lead to implant infraocclusion and open contacts. Implant occlusion and contact points need to be monitored over time. Knowing that these changes can occur will have a profound impact on restoration design. Key to long-term maintenance is predictable atraumatic retrievability such as occlusal or lingual screw retention even for single-tooth restorations. Implant occlusion with shallow incisal guidance protects implants from excessive lateral and tipping forces. One-piece full-arch restorations provide cross-arch stabilization and protection from eccentric forces. This type of restoration has the best chance to remain in function should an implant fail, provided that more than the minimum number of implants was placed.
ABOUT THE AUTHOR
Rainer H. Bergmann, DMD, Dr. med. dent.
Private Practice, Palm Desert, California
Queries to the author regarding this course may be submitted to authorqueries@aegiscomm.com.
REFERENCES
1. Kawanami M, Andreasen JO, Borum MK, et al. Infraposition of ankylosed permanent maxillary incisors after replantation related to age and sex. Endod Dent Traumatol. 1999;15(2):50-56.
2. Daftary F, Mahallati R, Bahat O, Sullivan RM. Lifelong craniofacial growth and the implications for osseointegrated implants. Int J Oral Maxillofac Implants. 2013;28(1):163-169.
3. Heij DG, Opdebeeck H, van Steenberghe D, et al. Facial development, continuous tooth eruption, and mesial drift as compromising factors for implant placement. Int J Oral Maxillofac Implants. 2006;21(6):867-878.
4. Op Heij DG, Opdebeeck H, van Steenberghe D, Quirynen M. Age as compromising factor for implant insertion. Periodontol 2000. 2003;33:172-184.
5. Fudalej P, Kokich VG, Leroux B. Determining the cessation of vertical growth of the craniofacial structures to facilitate placement of single-tooth implants. Am J Orthod Dentofacial Orthop. 2007;131(4 suppl):S59-S67.
6. Chee W, Jivraj S. Screw versus cemented implant supported restorations. Br Dent J. 2006;201(8):501-507.
7. Potashnick SR, Rosenberg ES. Forced eruption: principles in periodontics and restorative dentistry. J Prosthet Dent. 1982;48(2):141-148.
8. Brindis MA, Block MS. Orthodontic tooth extrusion to enhance soft tissue implant esthetics. J Oral Maxillofac Surg. 2009;67(11 suppl):49-59.
9. Klineberg IJ, Trulsson M, Murray GM. Occlusion on implants - is there a problem? J Oral Rehabil. 2012;39(7):522-537.
10. Klineberg I, Murray G. Osseoperception: sensory function and proprioception. Adv Dent Res. 1999;13:120-129.
11. Jacobs R, Van Steenberghe D. From osseoperception to implant-mediated sensory-motor interactions and related clinical implications. J Oral Rehabil. 2006;33(4):282-292.
12. Klineberg I, Kingston D, Murray G. The bases for using a particular occlusal design in tooth and implant-borne reconstructions and complete dentures. Clin Oral Implants Res. 2007;18 suppl 3:151-167.
13. Shemtov-Yona K, Rittel D, Machtei EE, Levin L. Effect of dental implant diameter on fatigue performance. Part II: failure analysis. Clin Implant Dent Relat Res. 2014;16(2):178-184.
14. Rangert B, Jemt T, Jörneus L. Forces and moments on Branemark implants. Int J Oral Maxillofac Implants. 1989;4(3):241-247.
15. Richter EJ. In vivo horizontal bending moments on implants. Int J Oral Maxillofac Implants. 1998;13(2):232-244.
16. Rangert B, Krogh PH, Langer B, Van Roekel N. Bending overload and implant fracture: a retrospective clinical analysis. Int J Oral Maxillofac Implants. 1995;10(3):326-334. Erratum in: Int J Oral Maxillofac Implants. 1996;11(5):575.
17. Cibirka RM, Razzoog ME, Lang BR, Stohler CS. Determining the force absorption quotient for restorative materials used in implant occlusal surfaces. J Prosthet Dent. 1992;67(3):361-364.
18. Ismail Y, Kukunas S, Pipko D. Comparative study of various occlusal materials for implant prosthodontics. J Dent Res. 1989;68:962.
19. Morneburg TR, Pröschel PA. In vivo forces on implants influenced by occlusal scheme and food consistency. Int J Prosthodont. 2003;16(5):481-486.
20. Kourkouta S, Hemmings KW, Laurell L. Restoration of periodontally compromised dentitions using cross-arch bridges. Principles of perio-prosthetic patient management. Br Dent J. 2007;203(4):189-195.
21. Priest G, Smith J, Wilson MG. Implant survival and prosthetic complications of mandibular metal-acrylic resin implant complete fixed dental prostheses. J Prosthet Dent. 2014;111(6):466-475.